Accidental extravasation of chemotherapy is a rare but feared complication of cancer treatment. Risk factors for extravasation include medication-related factors (such as the vesicant properties of the compound, or the volume, concentration, and duration of the infusion), patient-related factors (such as fragile veins, obesity, impaired consciousness, and lymphedema, and iatrogenic factors (including insufficient training, poor infusion technique, and use of improper cannulas).
Cancer chemotherapy is generally divided into three main classes according to vesicant potential, ranging from the high-risk vesicant drugs (eg, anthracyclines and vinca alkaloids) to irritants (eg, platinum compounds, topoisomerase I inhibitors, and taxanes) and the neutral drugs.
Clinical Manifestation
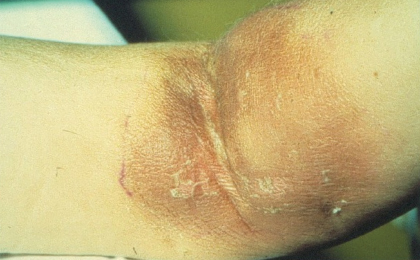
The clinical hallmarks of vesicant extravasations are acute pain, swelling, erythema, and a burning or tingling sensation. If left untreated, blistering may develop immediately or within days after the extravasation and may be followed by induration, discoloration, and, in severe cases, signs of tissue destruction (Fig. 1). After weeks to months, the slowly growing ulceration may invade and destroy deeper structures such as tendons and joints. The healing process is severely protracted, and a vesicant extravasation in an immunocompromised cancer patient is a major risk factor for bacterial colonization.
The resulting formation of scar tissue can contribute to long-term cosmetic and functional deficits. Treatment delay, termination of further planned chemotherapy, and even death from wound complications may be the ultimate outcome.
Treatment and Prevention
In the event of suspicion of an extravasation, the infusion should be promptly stopped, and attempts should be made to aspirate through the cannula. Areas of redness or edema should be marked and photographed for documentation.
The effects of anthracycline extravasations can be counteracted by prompt initiation of intravenous infusion of the systemic antidote, dexrazoxane. Depending on the type of the extravasated compound, the volume, and the area of extravasation, treatment options include cooling (or heating in cases involving vinca alkaloids), topical dimethyl sulfoxide, and subcutaneous hyaluronidase.
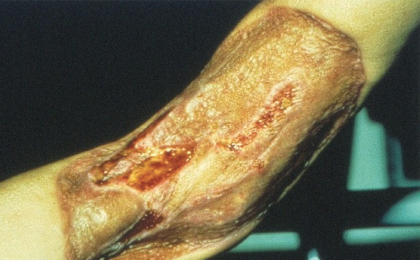
In selected cases, surgical tissue flushing with saline is used. In the event of necrotizing extravasation, surgical excision with wide margins and perhaps also skin grafting may be necessary (Fig. 2). Long-term follow-up includes treatment of cosmetic changes and the effects of nerve and muscle damage.
Extravasation is largely preventable by ensuring adequate education of the treating staff, information for patients, and use of proper injection techniques and remedies. International extravasation guidelines are now available and should also be available at an institutional level. ■
Disclosure: Dr. Langer reported no potential conflicts of interest.
Dr. Langer is Chief Physician and Head, Department of Thoracic and Neuroendocrine Oncology, Copenhagen University Hospital–Rigshospitalet, Copenhagen, Denmark.
Dermatologic Events in Oncology is guest edited by Mario E. Lacouture, MD, Associate Member in the Division of Dermatology, Department of Medicine, at Memorial Sloan-Kettering Cancer Center, New York. He is a board-certified dermatologist with a special interest in dermatologic conditions that result from cancer treatments.